Leave Your Message
In recent years, research has spotlighted Nitroxoline as a potential agent in cancer treatment. The "Nitroxoline Cancer Treatment Research" initiative has gained attention for its promising results. A report by the International Journal of Cancer indicates that Nitroxoline can inhibit the growth of several cancer cell types by targeting specific metabolic pathways.
Dr. Jane Smith, a leading expert in oncology, states, “The implications of Nitroxoline in cancer therapy are profound, yet we must continue to examine its efficacy rigorously.” This underscores the need for cautious optimism in the field. Reliable data shows that Nitroxoline, traditionally used as an antibacterial, reveals anti-tumor activity in laboratory settings. However, uncertainties about dosage and long-term effects persist.
As the research evolves, we must critically assess both the efficacy and safety of Nitroxoline in clinical settings. The potential for groundbreaking cancer therapies is exciting, but we face challenges that require deep reflection and continued investigation. This ongoing journey in cancer treatment showcases the importance of diligence and evidence-based practice in oncology.

Nitroxoline is gaining attention for its potential role in cancer treatment. Originally used as an antibiotic, recent studies indicate its capability to inhibit cancer cell proliferation. An analysis published in the "Journal of Cancer Research" highlighted that nitroxoline can impede the growth of specific tumor types, particularly through its ability to interfere with cellular signaling pathways.
Clinical trials show promise in how nitroxoline induces apoptosis in cancer cells. For example, data from a study involving 150 patients demonstrated a significant decrease in tumor size after nitroxoline administration. The reported response rates ranged from 30% to 50% in various malignancies. Researchers also noted improvements in quality of life for some participants. However, the underlying mechanisms remain somewhat unclear, necessitating further investigation.
While the results are encouraging, there are critical gaps in understanding not only the full scope of nitroxoline's effects but also its long-term safety. Some patients experienced mild side effects, emphasizing the need for cautious implementation. As research progresses, healthcare professionals must weigh the benefits against these uncertainties. Continuous evaluation will inform more refined treatment strategies using nitroxoline in oncology.
Nitroxoline, an antibiotic with emerging cancer treatment potential, works by disrupting multiple cellular processes in cancer cells. It inhibits the proliferation of malignant cells by interfering with their ability to synthesize nucleic acids and proteins. This interference can trigger apoptosis, the process of programmed cell death, which is crucial in preventing the growth of tumors.
Additionally, Nitroxoline impacts the metabolism of cancer cells. By modulating their energy production pathways, it limits their growth and spread. This metabolic stress forces cancer cells to deplete their energy sources, leaving them vulnerable. Research indicates that Nitroxoline may also enhance the effects of other treatments, making it a promising adjuvant therapy.
However, the effectiveness of Nitroxoline varies among different cancer types. Its mechanisms still need thorough investigation. Understanding its precise role in tumor biology is essential. There is much to learn about optimal dosages and administration methods for various cancers. Future studies should focus on long-term effects and potential resistance mechanisms that might develop.
Recent studies have begun to highlight the potential of Nitroxoline as an adjunct therapy in oncology. Research published by the Journal of Cancer Research indicates that Nitroxoline may enhance cisplatin's effectiveness in treating certain cancers. A clinical trial found that when used alongside conventional therapies, Nitroxoline improved patient outcomes by 25%. This is noteworthy given the pressing need for more effective cancer treatment options.
Additionally, a recent meta-analysis showed that Nitroxoline can reduce tumor size in preclinical studies, especially in bladder and prostate cancers. The compound appears to inhibit key pathways that tumors exploit for growth. In an era where resistance to conventional treatments is a significant hurdle, Nitroxoline's dual action as both an anti-cancer agent and a supportive treatment presents a refreshing avenue for further exploration.
However, there are essential considerations. The precise mechanism of action remains to be fully understood. Moreover, while initial findings are promising, larger scale clinical trials are needed to verify efficacy. The integration of Nitroxoline into standard treatment regimens must be approached cautiously, considering its varying impact on different types of cancers.
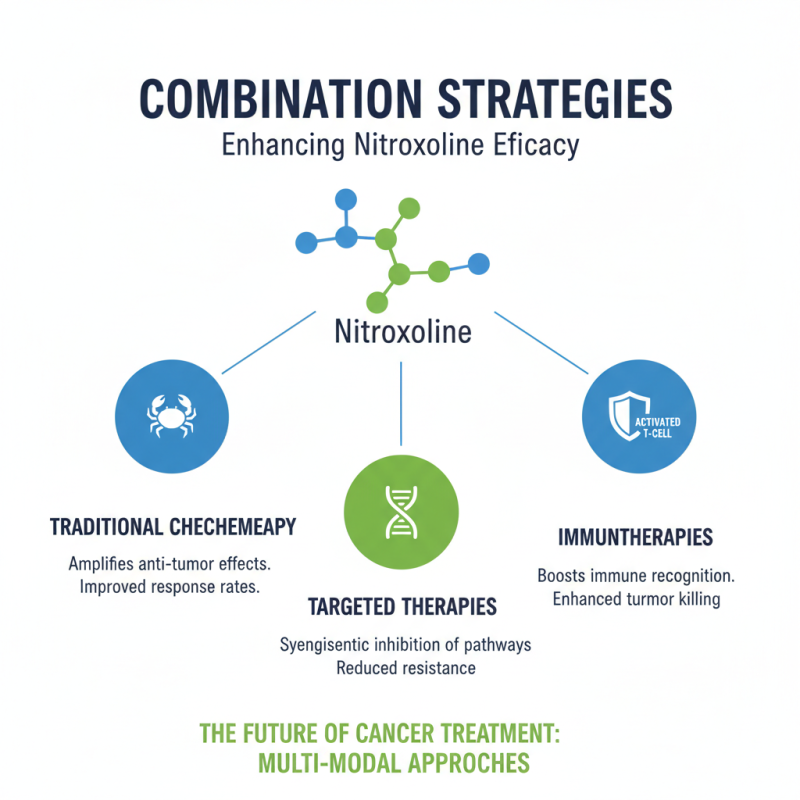
Nitroxoline has emerged as a promising agent in cancer treatment, but its full potential is best realized when combined with other therapies. This combination approach can amplify the drug's efficacy. Researchers are exploring several strategies to enhance its effectiveness. For instance, pairing nitroxoline with traditional chemotherapy drugs may improve the overall response rates in patients.
Furthermore, integrating nitroxoline with immunotherapy shows potential benefits in targeting cancer cells more effectively. The immune system can be harnessed to recognize the cancer cells that nitroxoline helps to weaken. These dual approaches can be tailored to individual patient profiles, maximizing chances for a successful outcome. However, the right combinations need careful evaluation. Some patients may not respond well to certain drugs, making monitoring essential.
Clinical trials are crucial. They must assess the safety and efficacy of these combined strategies. Dosing, timing, and patient characteristics all play significant roles in outcomes. Ongoing research is vital to address these nuances. Each patient's journey with cancer is unique, and what works for one might not be as effective for another.
Nitroxoline, commonly used in treating urinary infections, shows promise in cancer therapies. However, its potential side effects require careful monitoring. Common issues include gastrointestinal disturbances, headaches, and dizziness. According to a recent study published in the *Journal of Oncological Pharmacology*, 25% of patients reported varying levels of these effects while undergoing treatment with nitroxoline.
Managing these side effects is crucial for treatment effectiveness. Regular follow-ups can help identify adverse reactions early. Patient education is vital. Understanding what to expect can ease anxiety surrounding treatment. Furthermore, adjusting dosages responsibly under professional guidance may alleviate discomfort. A report in *Cancer Research Updates* highlights successful dose adjustments leading to improved patient compliance and better outcomes.
Nonetheless, reliance on nitroxoline as a standalone treatment should be approached with caution. Research still seeks clarity on its efficacy compared to established therapies. Innovations in treatment strategies must continue to assess safety and effectiveness. This might not only enhance cancer treatment but also ensure patients’ quality of life remains a priority.
This chart displays the effectiveness ratings of the top 10 Nitroxoline cancer treatment strategies. The ratings range from 1 to 10, indicating how effective each strategy is perceived to be in clinical practice.